Full article
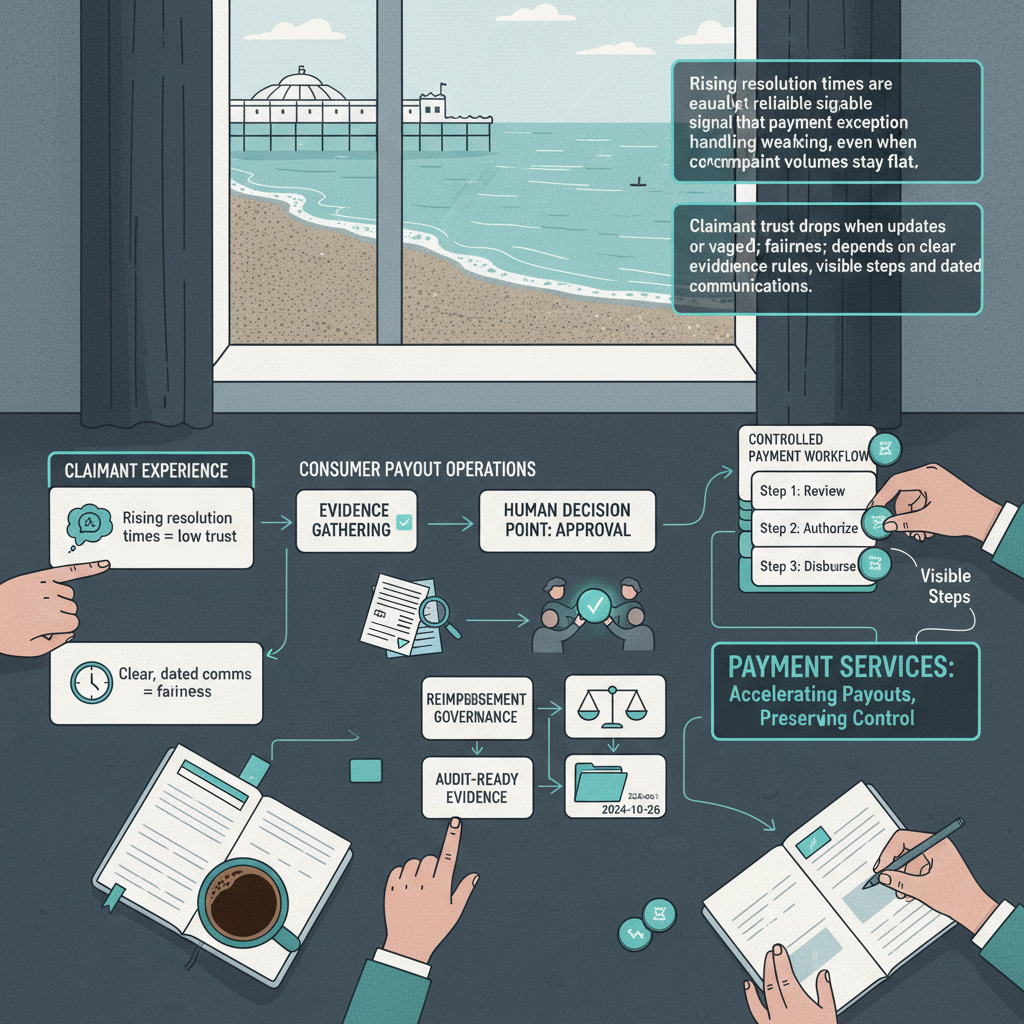
Executive summary: When a standard payment journey fails, the exception process becomes the product. That is where claimant trust is won or lost. In healthy consumer payout operations, exceptions have clear owners, evidence rules, dates and an audit trail. In weaker setups, they bounce between Care, Finance and Compliance until someone gives them a shove.
The signal is usually boring before it becomes expensive: resolution times drift up, update quality drops, and more cases need manual intervention. This note looks at those signals, what they imply for reimbursement governance, and the practical actions that put the process back on a path to green.
Signal baseline
The first sign of trouble is rarely a spike in complaints. It is a slower queue. In Q4 last year, on a retail programme review, average time-to-resolve for payment-related tickets moved from two business days to more than five, even though exception volumes were broadly steady. That matters because the process had not become busier; it had become weaker.
The pattern was familiar. Consumer Care received the issue, Finance checked payment status, Compliance reviewed edge cases, then someone had to chase for an answer. Each handoff added delay and diluted ownership. I was wrong about the effort at first; I assumed the root cause was training. The data pointed elsewhere. The real issue was a porous workflow with too many manual steps and no shared acceptance criteria.
That creates a measurable cost, not just a bad feeling. In that same review, each manual exception consumed roughly 45 minutes of combined staff time across three teams. At a few hundred cases a month, that is a decent chunk of operational capacity gone on preventable admin. If your plan cannot tell you who owns the case, what evidence is missing, and by when the next update is due, it is not a plan, fix it.
What is shifting in the claimant experience
Claimants do not expect perfection. They do expect clarity. Once someone has reported a failed payment and submitted evidence, silence becomes the problem faster than the original transaction does. A holding line such as “we are looking into it†buys you very little if there is no date for the next update and no clear route to decision.
That links directly to fairness. CAP and ASA guidance on promotions is clear on the basics: mechanics, conditions and outcomes should be understandable, auditable and not overstated. The same operational principle applies to exception handling. You should not make the claimant guess how a decision will be made, what evidence is needed, or whether anyone is actually dealing with it. Fairness in this context is not theatre. It is a visible process with sensible checkpoints.
Yesterday, after stand up, ticket PAY-2026-045 was blocked by an evidence query on a £50 goodwill payment. A quick call with Jane in Care and Mike in Finance cleared it, and a new decision date was set for 29 April 2026. Useful in the moment, but the signal was bigger than the ticket. The blocker existed because “sufficient evidence†had never been defined properly. Between 10:00 and 11:30, I rewrote the acceptance criteria for that payment story, tests passed once duplicate receipt imagery was covered, and Compliance took the action to formalise the rule set by 30 April 2026. That is the bit worth keeping.
Where ownership usually breaks
Most weak exception flows suffer from distributed accountability. Care owns the conversation. Finance owns the disbursement. Compliance owns the audit trail. Legal may appear if the case is awkward. Everyone owns a slice; no one owns the end-to-end outcome. The result is predictable: slower cycle times, inconsistent claimant messaging and patchy evidence records.
For reimbursement governance, the fix is not complicated, though it does require a decision. One named operational owner should be accountable for the measure that matters most: ticket opened to claimant paid, or ticket opened to claimant declined with reason logged. Finance should retain financial controls. Compliance should define required evidence and retention rules. But Operations should own flow, queue health and escalation dates. Otherwise, you are managing queues rather than a service.
Tooling exposes the same weakness quite quickly. A shared spreadsheet is not a controlled payment workflow. It cannot reliably enforce states, maintain secure evidence handling, or give you an audit-ready action log. The minimum workable setup is modest: status-controlled case management, named stage owners, timestamps, and immutable notes showing who did what and when. That can be a configured case tool or a disciplined Jira workflow. It does not need to be flashy. It does need to be traceable.
What good looks like in practice
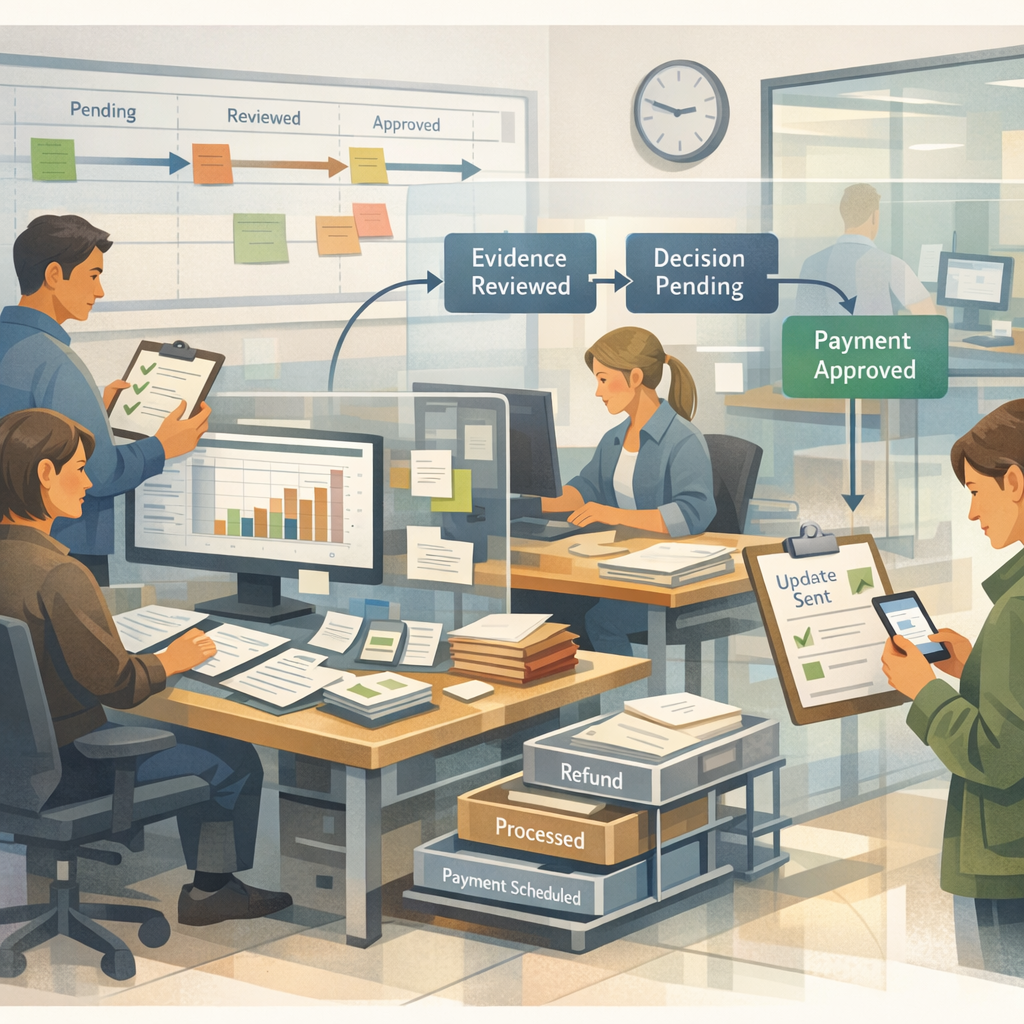
A sound exception process is testable. It has entry criteria, routing rules, approval thresholds, and a defined claimant communication pattern. It also makes the consumer path easy to understand: issue raised, evidence checked, decision made, payment released or declined, claimant informed. No hidden steps, no performative complexity.
For consumer payout operations, there are a few checkpoints that tell you whether the design is holding up. First, median time-to-resolution should be visible by exception type and value band, reviewed weekly by the process owner. Second, first-response and next-update service levels should be explicit, for example an initial human update within one business day and every two business days after that until closure. Third, exceptions resolved without cross-team rework should trend up once evidence thresholds are published. If that metric does not improve, your acceptance criteria are still too vague or your routing is wrong.
You also need a fair claim and distribution pattern. That means the claimant understands what they need to provide, what happens next, and how a payment is approved without arbitrary judgement. If the process relies on someone remembering a precedent from six months ago, you are one holiday away from inconsistency. Bit tight on time is not a control.
Actions and watchpoints for Q2 2026
Here is the practical plan. It is deliberately plain because plain plans survive contact with reality better.
- Map the unhappy path by 30 April 2026. Owner: Head of Operations. Run a 90-minute workshop with leads from Care, Finance and Compliance. Acceptance criteria: one signed-off process map covering every step from claimant contact to payment confirmation or decline; all handoffs named; all systems listed; current decision points and rework loops marked. Risk: teams document the ideal process rather than the actual one. Mitigation: use ten recent live cases as evidence during the session.
- Publish evidence thresholds by 15 May 2026. Owner: Head of Compliance. Define the minimum evidence needed for refunds, reimbursements and goodwill payments by value band, including edge cases such as duplicate receipts and partial bank details. Acceptance criteria: a version-controlled guide available to Care and Finance; escalation triggers defined; change log in place. Risk: rules become too rigid and increase decline rates. Mitigation: include an override path with named approvers and a reason code.
- Pilot a lightweight workflow tool by 30 June 2026. Owner: Head of Delivery. Configure stage-based routing, SLA prompts, audit logs and claimant update templates. Acceptance criteria: 100% of new exception cases logged in the tool; average time-to-resolve reduced to under 48 hours for in-scope cases; no spreadsheet used as the primary tracker by pilot end. Risk: teams continue to work offline. Mitigation: daily review of off-system cases for the first two weeks and weekly exception reporting after that.
There is one open decision to force through, because it affects both speed and control. The threshold for Care to resolve low-value cases without extra approval is still under debate: Finance prefers £10, while Care argues £25 would cover close to 80% of common issues on first contact. Fine. Make it a test, not a philosophical argument. Assign the decision to the steering group, review by 22 May 2026, and measure error rate, rework rate and claimant satisfaction over a four-week pilot. Cheers, sorted.
The operational implication
Weak payment exception handling does not stay hidden for long. It shows up as wasted staff hours, slower decisions, harder audits and a claimant experience that feels arbitrary. The organisations that handle this well do not rely on heroic individuals. They use clear ownership, dated actions, acceptance criteria and a system that keeps the evidence straight.
If your team is seeing resolution times drift, repeated evidence disputes, or too many cases trapped between Care and Finance, that is the point to intervene. Holograph helps teams design consumer payout operations that are faster for claimants, tighter for Finance, and easier to defend under scrutiny. If you want a practical review of your current exception flow, contact Holograph and we will map the weak points, assign owners, and give you a realistic path to green.
If this is on your roadmap, Holograph can help you run a controlled pilot, measure the outcome, and scale only when the evidence is clear.



